When you visit a doctor because of back pain, they will run a series of tests to get a clear picture of your spine. Not only do these tests confirm their diagnosis, but they also help your doctor understand the severity of your condition. They can see whether your pain is caused by one slipped disc or if there are multiple degenerating discs that are limiting your range of motion.
One test that doctors rely on in particular for spinal imaging is a magnetic resonance imaging (MRI) scan. If your doctor suspects that you have a herniated disc, they will ask you to get an MRI to confirm their theory.
Even the most experienced surgeons use MRIs and other imaging tests to diagnose patients. These images can tell doctors exactly where the problem disc is located and how it should be approached. Dr. Todd H. Lanman, a board-certified spinal neurosurgeon, relies on MRIs to determine whether a damaged disc could potentially heal on its own or if it needs surgical intervention. With more than 30 years of experience, he can quickly review MRI scans and develop individualized treatment plans.
Learn more about getting an MRI and what a herniated disc looks like on these scans. Getting the right imaging tests is the first step toward healing your back pain.
What Is a Herniated Disc MRI and When Do You Need One?
When you visit the doctor because of back pain, they will try to identify whether the cause is related to your spine. If so, your doctor will ask you to get an MRI. With the right imaging, they should be able to see if any discs are herniated and the severity of their movement into your nerve canal.
Understanding Herniated Discs
A herniated disc is sometimes referred to as a slipped or bulging disc, depending on how the disc itself is protruding. It occurs when one of the spinal discs that protect your vertebrae gets pushed out of place or if the jelly center that works as a shock absorber (known as the nucleus) pushes through the outer wall (the annulus). Herniated discs can be caused by trauma – like a sports injury or car accident – or can develop naturally with age.
Some patients don’t realize they have a herniated disc because it isn’t pushing into their nerve canal. However, when the disc starts to hit your nerves, it can cause a variety of uncomfortable symptoms. These include:
- Chronic pain, either in the form of a dull, throbbing ache or unexpected, sharp twinges.
- Numbness or tingling in the extremities, either in the arms for a cervical herniation or the legs for a lumbar herniation.
- Reduced range of motion because the pain prevents you from moving comfortably.
- Weakness in the arms or legs.
These symptoms can get worse if the herniation goes untreated and is unable to heal on its own. The pain might be more severe or more frequent depending on the patient.
An MRI can provide a clear image of the herniated disc so doctors understand how to treat the source of discomfort. Patients might be able to treat their herniations with physical therapy, medication, and hot and cold compresses before they need to consider surgery.
Herniated Discs and MRI Images
Modern MRIs provide clear images of the human spine. Not only can doctors see which disc is affected, but they can also understand why it is causing you so much pain. This helps them develop a treatment plan to slow the progression of the slipped disc so your condition doesn’t get worse. Here are a few MRI images and the types of information they convey.
Visualizing Disc Protrusion on MRI
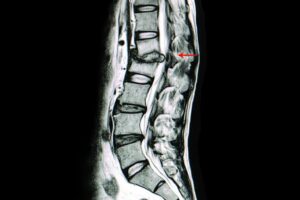
This image allows you to see what a protrusion looks like compared to normal spinal discs. Each disc along the spine provides a cushion between the vertebrae and allows the back to curve naturally. One spinal disc has fallen out of place and is pushing into the nerve canal. You can also see how the slipped disc puts the two vertebrae at risk of knocking against each other –- causing additional discomfort to the patient.
If a doctor saw an MRI like this one, they could immediately see the source of the patient’s discomfort and how the pain could be addressed.
Nerve Compression
A pinched nerve occurs when there is too much pressure placed on a nerve because of surrounding tissue. It can occur throughout your body but is common with herniated discs. In this case, the slipped disc puts pressure on the nerves that run up and down your spine.
With this image, you can see the nerve canal as a singular tube that is parallel to your spine. The herniated disc is pushing against the nerve and causing it to compress against the rest of the body. Because nerves carry information to the body’s extremities, nerve compression in one part of the spine can cause numbness or tingling in your fingers or toes.
Structural Changes and Disc Degeneration
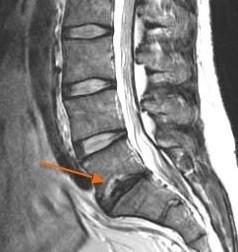
There are times when disc degeneration can lead to herniation. Degeneration occurs when a spinal disc breaks apart or wears out, which can then cause it to slip out of place.
Using the image above, you can compare the degenerative disc to the healthy discs above it. The healthy, white discs are hydrated, intact, and staying in place. The degenerative disc doesn’t provide any structural support and is slipping into the nerve canal.
While many herniated discs can heal on their own, degenerative discs often cannot. For a severe case, a doctor might recommend removing the broken disc and replacing it with an artificial model (known as total disc replacement surgery) that provides support and stays in place.
Dr. Todd Lanman’s Perspective: Interpreting MRI Findings
Dr. Lanman frequently asks patients to get MRI scans if he suspects that they have herniated discs. This allows him to make informed decisions about their back pain while tracking their progress as he prescribes different treatments.
When a specialist looks at herniated disc MRI results, there are a few key things they look for. These include:
- The health of the spinal disc. Is it only herniated or are there signs of degeneration?
- If the spinal disc is intact. A herniation could be a simple protrusion or it could be an extrusion if the inner nucleus has broken through the outer wall (annulus).
- The impact of the herniation on the nerve canal. This is often the cause of pain in patients. A disc herniation could lead to nerve compression that needs to be addressed.
- How the herniation affects the rest of the spine. Degeneration or severe herniation can cause the vertebrae to knock against each other, causing additional pain.
By going through this checklist when reviewing an MRI scan, Dr. Lanman will be able to suggest a course of treatment that is relevant to the patient’s needs. In many cases, this will involve non-invasive options to help the herniation heal on its own. However, if there is severe degeneration or the nerve canal is significantly affected, Dr. Lanman might recommend artificial disc replacement to immediately address the issue.
An MRI Can Help You Get the Treatment You Need
An MRI is a painless test that helps doctors diagnose a variety of conditions, including herniated discs. During the MRI scan, you can lie back and let the magnetic imaging do the work. This is often considered a painless test for patients.
If you experience back pain, don’t hesitate to visit a spinal specialist. An expert surgeon like Dr. Lanman will quickly be able to identify the cause of your discomfort and develop a treatment plan. Dr. Lanman is a quality resource if you want personalized care and an experienced doctor to support you. Learn more about herniated discs and request a consultation with Dr. Lanman today.
FAQs
How is an MRI different from other imaging techniques for herniated discs?
An MRI is considered the best possible tool for looking at spinal discs. The main difference between an MRI and an X-ray or a computed tomography (CT) scan is that an MRI can look at soft tissue, not just bones and joints. This provides far greater detail to the doctor who looks at the scans and makes it easier for patients to understand the source of their back pain.
What are the main causes of a herniated disc?
There are two main ways to sustain a herniated disc. The first is through unexpected trauma or an injury – like a car accident. This forcefully pushes the disc out of place. The next way to get a herniated disc is through age. Your spinal discs can start to wear out over time, which makes older people more likely to develop this condition.
Can a herniated disc be diagnosed without an MRI?
In most cases, your doctor will order an MRI to look at your spine. However, they might also get the information they need from a CT scan. Even if your doctor is confident that you have a herniated disc, they still need to run these tests to confirm their diagnosis. These tests can also help your doctor track the progress of your healing over time.
What are the risks associated with herniated disc surgery, including artificial disc replacement?
Disc surgery is considered a minimally invasive procedure that can be completed in less than an hour. However, every operation comes with risks. There’s a chance that your body might reject the artificial disc or have an allergic reaction to it. There also is no guarantee that your pain completely goes away. However, this operation has high success rates and the risks that come with it are very low.
How long does it take for a herniated disc to heal without surgery?
Most herniated discs heal by themselves and do not require surgery. If you follow your doctor’s recommendations and rest your spine, you should heal your herniation within six weeks. However, if you continue to participate in strenuous activities (like standing all day and lifting heavy objects), then your herniation will take longer to heal.
Ready to reclaim your life? Get in touch with Dr. Lanman Today.
FOLLOW US ON SOCIAL MEDIA | @ADRSPINE





